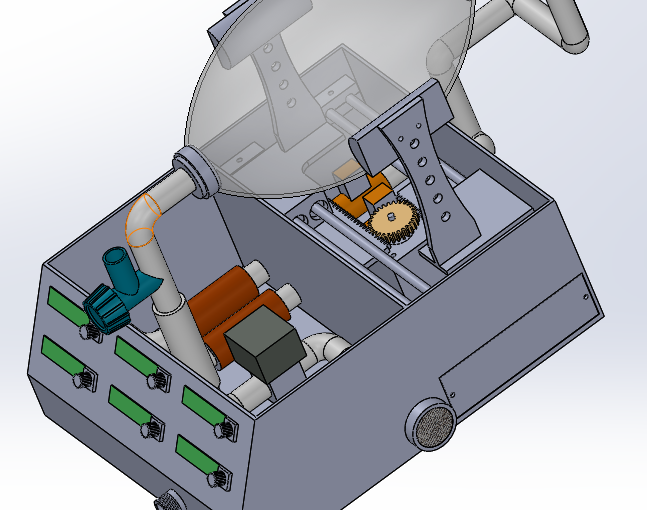
Our Solution
- With lack of Ventilators vs the numbers of the victims of COVID 19 and the high cost of it. so we need to build a low cost Ventilators to support our countries in the middle east.
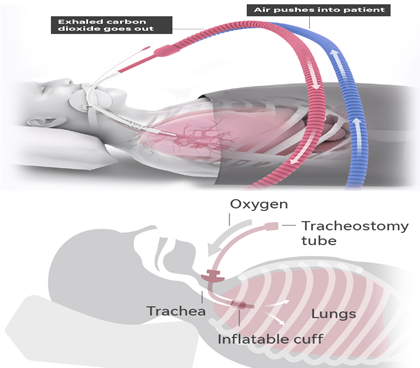
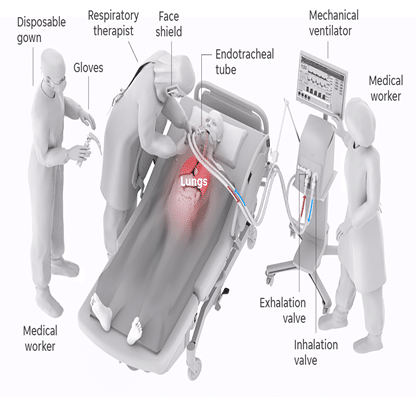
- Ventilators gently pump air through a breathing tube into the patient’s lungs and allow the patient to exhale. This gives patients oxygen and removes carbon dioxide, which can damage the patient’s organs if not expelled. In some cases, air with higher oxygen content is used. Settings are tailored to patient needs.
- Patients can’t talk because the tube passes through their vocal cords. The tubes can be uncomfortable and it takes time to get used to them, according to AgingCare.
- Ventilator operation is closely monitored to maintain pressure and expiration levels.
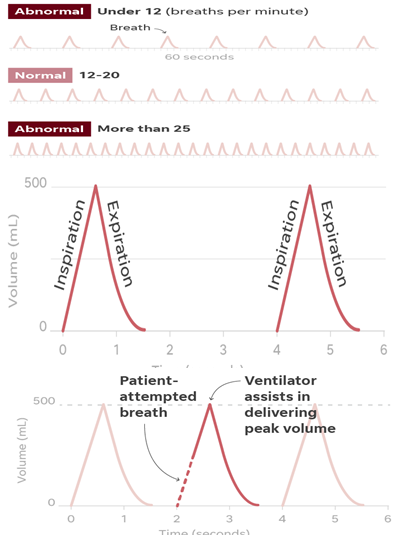
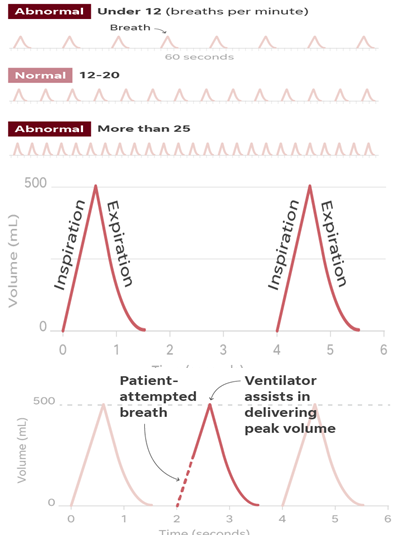
- Doctors monitor patient breathing rates per minute.
A popular mode used with ventilators is called assist-control (AC). In that mode, the ventilator assists with breathing. It’s ideal for recovery because the patient only has to initiate a breath and the ventilator does the rest.
In this example, the respiratory rate is set to 15 breaths per minute. That means the patient will receive a breath every four seconds, regardless if the patient needs a breath.
Even if the patient attempts a breath in between the timed breaths, the ventilator will take over and deliver the same volume of air as the timed breath. - Patients are connected to ventilators in three ways. Though patients are sedated for the invasive procedures, the process of putting tubes in patients can be dangerous for health care workers, who risk being infected themselves. There’s also a risk of infection for patients with breathing tubes.
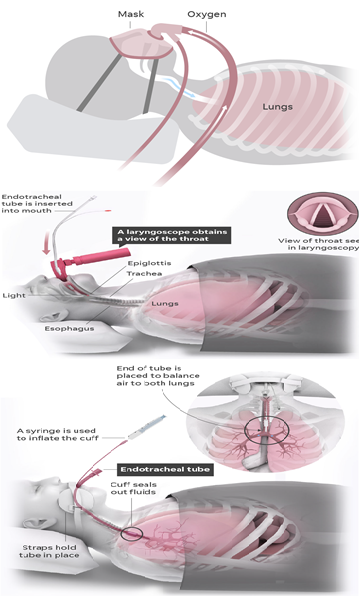
- Non-invasive mask:
In less critical cases, oxygen can be delivered through a face mask instead of a tube. This type of ventilator can be more commonly available in some areas and is relatively safe to deploy. - Endotracheal tube:
For more invasive procedures, medical workers don protective clothing and sanitize and sterilize the ventilator equipment.
A specialist called a respiratory therapist inserts a laryngoscope into the patient’s mouth and guides the endotracheal tube into the windpipe.
Once the tube is inserted, a cuff is inflated to keep the tube in place and seal out secretions. The laryngoscope is removed and the tube is taped to the side of the face. The tube is checked to make sure it can equally inflate both lungs.
The endotracheal tube is attached to the lines running to the mechanical ventilator.
Endotracheal tube
The endotracheal tube is attached to the lines running to the mechanical ventilator - Tracheotomy:
This is a more invasive procedure with an incision in the windpipe for insertion of a tracheal tube. This method is less likely to be used for COVID-19 patients since it puts the health care team at increased risk from aerosolized viral particles which can remain infectious for up to three hours.





Highly advise you to apply to the COVID19 Detect and Protect Challenge by Hackster.io and UNDP: https://www.hackster.io/contests/UNDPCOVID19
الروابط جميعها لاتعمل للأسف